Diagnostic Testing and Evaluation
People with bronchiectasis and/or NTM lung disease may be asked to do a series of tests, depending on the reason for their visit to the doctor. Some tests, such as CT scans, are used to diagnose bronchiectasis. Other tests, such as pulmonary function tests (PFTs), are used to tell us how well the lungs work. These diagnostic tests and evaluations give health care providers important information that will be used to decide the best course of treatment for the patient. Results of these tests can highlight the extent of lung damage (if any); the location (within the lungs) of the disease; the type(s) of bacteria that may be growing in the lungs; the type(s) of antibiotics that may be effective in treating the disease; and the patient’s lung function level. This information will also be used in the long-term management of the disease, as it will allow the health care provider to watch how the disease may progress over time. This type of long-term disease management can be helpful in preventing exacerbations (flare-ups), improving symptoms, and maintaining patients’ quality of life.1
Chest X-ray
On initial evaluation, a doctor may order a chest X-ray, which is one type of imaging. Chest X-rays are simple, painless, and quick pictures of the lungs. Chest X-rays are not used to diagnose bronchiectasis or NTM lung disease but are generally done to rule out other chronic lung diseases or sudden illnesses or injuries. (e.g., pneumonia or bronchitis).2
Preparing for a chest X-ray
- Before the chest X-ray, you will be asked to take off any jewelry from the waist up. Also, you may be asked to put on a patient gown.
- For the chest X-ray, you will stand in front of a flat panel (and may be asked to turn and face different directions or hold your arms up in the air in order to capture several different views of your lungs).
- The technician will stand across the room and point a piece of machinery (shaped like a tube) toward you to take the X-ray.
- When the X-ray is done, follow up with your doctor to discuss the results of your chest imaging.3
- Many people find it helpful to ask for a copy of their chest imaging on a disc so that they can share the actual study pictures with their health care providers and keep a copy for their own records.
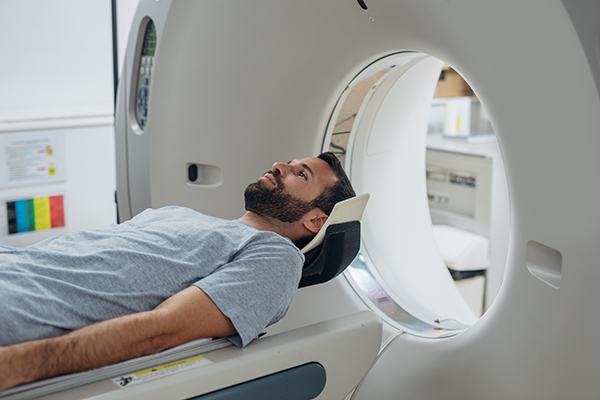
High Resolution Chest Computerized Tomography (HRCT)
An HRCT, also known as a high-resolution CT scan, is a special type of CT scan. In this type of chest imaging, a computer takes “slice-like” images of the lungs to give a detailed picture of what the lungs look like from top to bottom. The difference between an HRCT and a normal CT scan is that in an HRCT, additional images are often obtained, and the images are later analyzed by a special computer program to show even more detailed information about the appearance of your lungs. While a normal CT scan may be good enough to make a diagnosis of bronchiectasis for some patients, HRCT is considered the gold standard for the diagnosis and description of bronchiectasis.
On chest imaging, bronchiectasis is seen as a permanent widening of the bronchial airways. Radiologists measure the location and amount of this widening and compare it to the size of the blood vessels in the lungs. Other important chest imaging results in people with bronchiectasis are thickened airway walls and areas of mucus plugging (mucus collecting in one place).1
Getting ready for your HRCT
- Wear clothing that you can take off from the waist up. You may be given a gown to wear during the test. You will need to take off all jewelry from the waist up.
- The HRCT will not hurt. Before the scan, the radiology technician will explain what to expect during the scan. Ask questions if you do not understand.
- The total time of the test may vary between 5-20 minutes, as both getting you ready and making sure you are in the right position are important. During this time, you will lie flat on your back on a table as it moves back and forth through the scanner. At times you may be asked to raise your hands above your head and hold your breath for several seconds. It is important that you follow all directions from the radiology technician and stay as still as possible. For some tests you may also be asked to lie on your stomach for a brief time.
- After the HRCT is complete, follow up with your doctor to talk about the results of your chest imaging.3
- Many patients find it helpful to ask for a copy of their chest imaging on a disc so that they can share the actual pictures with their health care providers and keep a copy for their own records.
Pulmonary Function Tests (PFTs)
PFTs are different breathing tests that can help to measure how well the lungs work. These tests (or series of tests) are given by respiratory therapists or specially trained health care providers. During the testing, the patient is told to take deep breaths and blow hard into a measuring device. PFTs are painless, but patients may feel tired or slightly breathless after the test, especially because sometimes the test needs to be done several times to make sure the results are the same each time.
Doctors order PFTs to look at how severe airflow obstruction (narrowing or blockages of the airways) is in patients with bronchiectasis and NTM lung disease. In bronchiectasis and NTM lung disease diagnoses, clinicians take a close look at measurements like forced expiratory volume in the first second (FEV1), forced vital capacity (FVC), and peak expiratory flow rate (PEF).1 Your disease can change your results over time and can sometimes be a sign of risk for flare-ups and hospital admission.1 Repeated testing over time is often recommended to track your lung function.
Getting ready for PFTs
- Prior to your PFTs, read all instructions given to you. You may be asked to stop your breathing medications for a day before the test.
- The PFTs can include a different breathing tests such as spirometry (how much air you can breathe in and out), lung volumes (information on how your lungs are functioning), and diffusion capacity (how well you move oxygen from the lungs to the blood), among other tests. The PFT technician will let you know which breathing test(s) you will be given.
- Before starting the test, the technician will place a soft clip on your nose.
- During the test, the technician will coach you to get the best results from each test. It is important to give your best effort in order to get the best results. You may be asked to do each test several times.
- You may be asked to sit in a plastic booth called a body box (or plethysmograph). In this booth, you will be asked to do several different breathing tests. Talk to your PFT technician if you suffer from claustrophobia (a fear of closed-in spaces) or have a fear of being in small spaces.
- For some types of PFTs, during your testing you may be given an inhaled medicine that opens your airways, such as albuterol, and then have the testing done again to see if this medicine improves your lung function.
- The full group of PFTs may take up to one full hour to finish.
- After your PFTs, follow up with your doctor to talk about the results of your testing.

Sputum Culture
Bronchiectasis has different impacts on different patients. Some patients with mild bronchiectasis have a dry cough but may not create much mucus every day. However, other patients with moderate to severe bronchiectasis usually produce mucus in moderate to large amounts.1 A sputum culture is a test used in those with lung infections to see what type(s) of bacteria (if any) are in the mucus that is coughed out. When a lab can find out the type(s) of bacteria that are in your mucus, your doctor can decide if antibiotics are needed and, if so, which ones will be helpful in treating the infection. Pseudomonas aeruginosa and NTM are two types of bacteria known to cause lung infections in people who have bronchiectasis.
Getting ready for a sputum culture
- A small sterile plastic cup will be given to you by your doctor or by your laboratory for sputum collection.
- You may be asked to take the cup home for collection when you are able to cough up mucus.
- As the inside of the cup is sterile (or completely clean), do not break the seal on the cup until right before you are ready to produce mucus for collection.
- In order to produce a good quality sample for testing, it is important to collect mucus (from the lungs) rather than spit (from the mouth).
- Often times the best time to collect a high-quality mucus from your lungs is in the morning.
- Once you can cough up the mucus from your lungs, you will bring the sample to the doctor’s office or lab for testing.
- If you are not able to cough up any mucus, you may be asked to use a nebulizer containing hypertonic saline to help cough up mucus, which is a process called sputum induction. Simply put, saline is salt water. Hypertonic saline has a higher concentration of salt.
- The basic results of the sputum culture should be ready for your doctor to review in about two weeks; however, some results (including mycobacterial cultures) can take up to two months.6
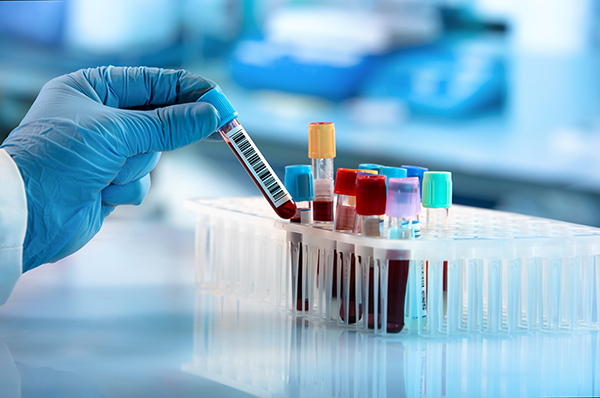
Blood Test
Blood tests are a very common tool doctors use to diagnose many diseases. A blood test may be ordered by your doctor to tell them about your general health, how your immune system works, and to possibly discover the cause of your bronchiectasis.7
Getting ready for a blood test
- For many blood tests, no special preparation is needed. There are a few tests that may require the patient to not eat for 8-12 hours. Your doctor will let you know ahead of time if not eating is necessary, but that is generally not required for the much of the blood testing done related to NTM lung disease or bronchiectasis.
- During the blood test, a small sample of blood is taken from the body using a needle. It is typically drawn from a vein, but sometimes a finger prick will be used.
- Although the patient may feel some discomfort from the needle, the blood test is quick.
- Most people do not have any serious reactions; however, if you have a lot of bruising, you should tell your doctor.8
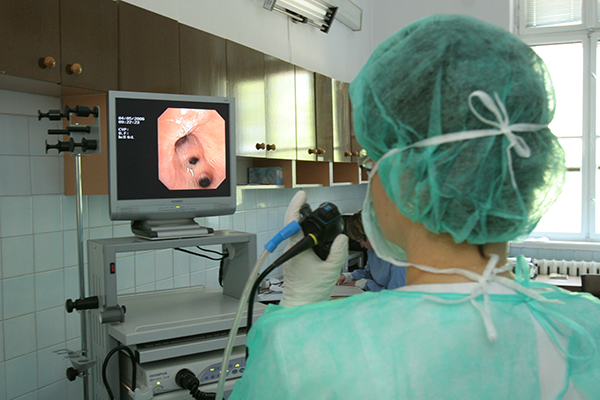
Bronchoscopy
In some cases, your doctor may do a bronchoscopy as part of the evaluation of bronchiectasis and NTM.9 A bronchoscopy is a test that allows your doctor to look at the inside of your lungs using a bronchoscope. A bronchoscope is a thin, flexible tube with a camera on the end that can be put into the lungs to help find blockages or look for signs of infection. The camera is often linked to a video screen where the doctor can record and take pictures of your airways. During bronchoscopy, your doctor can also take samples, including washings of the lung or biopsies of lung tissue that can be tested later in a lab.
Getting ready for a bronchoscopy
- You will be asked to not eat after midnight the night before your test. If you take daily medicines, talk to your doctor before your appointment about which ones they want you to take. For instance, you may be asked to stop taking certain blood thinners for a few days before the test.
- The medicines they give you during the test may make you groggy for several hours afterward. Plan for a friend or a loved one to drive you home after the bronchoscopy.
- You will be asked to sign a form prior to the bronchoscopy. This form will tell you about any possible risks. Make sure you ask your doctor any questions that you may have.
- Typically, bronchoscopies do not require general anesthesia. However, your doctor will give you medicine to relax you prior to the test. The health care workers helping your doctor may also use numbing sprays or gels to lessen any discomfort you may feel.
- Your vital signs – such as heart rate and blood pressure – will be watched throughout the test.
- Overall, the test will last between 30 minutes and one hour.
- After the bronchoscopy, you may have a sore throat, hoarseness, and/or a cough. These should go away after a couple of days.
- Your doctor will schedule a follow-up appointment to talk about findings and results from any testing done on samples taken during the bronchoscopy.10
Six-minute walk test (6MWT)
This is a walking test that is performed to find out a patient’s level of fitness and possible need for oxygen therapy while doing activity.11 During this test, your health care provider may need to add or increase supplemental oxygen by watching your oxygen levels using a pulse oximeter. A 6-minute walk test is painless, but depending on a patient’s level of fitness, they may feel tired afterward.
Getting ready for a 6-minute walk test
- Wear comfortable clothing and shoes. Avoid sandals, flip flops, high heels, or slippers.
- Keep taking all your medicines that day as prescribed.
- Eat a light meal 1-2 hours before your test.
- If you have diabetes and activity tends to affect your blood sugar, bring your glucose monitor, test strips, and have a snack available if your glucose should drop.
- Before, during, and after the test, your heart rate and oxygen levels will be checked with a pulse oximeter. Remove any dark nail polish from your nails in order to get a fast and reliable reading.
- Let the staff know if during the test you feel chest pain or find it hard to breathe.
- The walking portion of the test will last six minutes, but the total testing time will last at least 30 minutes for proper monitoring before and after the 6-minute walk.12
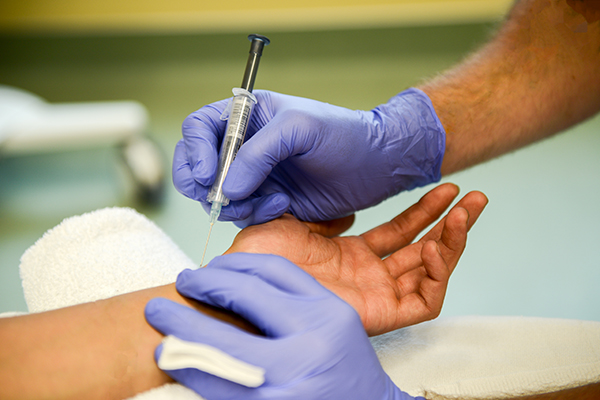
Arterial Blood Gas (ABG)
An ABG is a needle puncture that is done by trained health care workers. Commonly, the needle puncture will be done on the radial artery (in your wrist), but (in some cases) arterial puncture may be done on the brachial (inside elbow) or femoral arteries (near the groin). Arterial blood gas testing is done to help assess treatment, indicate the severity of a condition, or it can be used to evaluate long term use of oxygen therapy.12 The results of the ABG will tell your doctor how much oxygen and carbon dioxide are in the arterial blood as well as several other parameters.12
Getting ready for an ABG
- The ABG will be drawn at the pulse site on the wrist. A quick test will be done by the technician to make sure there is good blood flow to the hand.
- You may feel some discomfort as the needle is gathering the blood sample.
- After the sample is collected, the person drawing the blood should put pressure on the site for 3-5 minutes.
- Tell your doctor if you have a large amount of bruising after an ABG.13
References
1Chalmers JD, Sethi S. Raising awareness of bronchiectasis in primary care: overview of diagnosis and management strategies in adults. NPJ Prim Care Respir Med. 2017;27(1):18. Published 2017 Mar 13. doi: https://doi.org/10.1038/s41533-017-0019-9
2Breathe. Bronchiectasis | European Respiratory Society (ersjournals.com). https://breathe.ersjournals.com/content/14/1/73. Accessed March 26, 2021.
3National Jewish Health. Chest x-ray. https://www.nationaljewish.org/conditions/tuberculosis-tb/diagnosis/chest-x-ray. Accessed March 29, 2021.National Jewish Health. CT scan of the chest.
4National Jewish Health. CT scan of the chest https://www.nationaljewish.org/conditions/tests-procedures/imaging/ct-scan-chest. Accessed March 29, 2021.
5National Jewish Health. Routine pulmonary function test. https://www.nationaljewish.org/conditions/tests-procedures/pulmonary-physiology/pulmonary-function/routine-pulmonary-function-test. Accessed March 29, 2021.
6National Jewish Health. Sputum Test. https://www.nationaljewish.org/conditions/tuberculosis-tb/diagnosis/sputum-test. Accessed March 30, 2021.
7The European Lung Foundation. Bronchiectasis. Breathe. 2018 14: 73-80; DOI: https://doi.org/10.1183/20734735.ELF141
8National Heart, Lung and Blood Institute. Blood tests. https://www.nhlbi.nih.gov/health-topics/blood-tests. Accessed March 31, 2021.
9American Lung Association. Bronchiectasis symptoms and diagnosis. https://www.lung.org/lung-health-diseases/lung-disease-lookup/bronchiectasis/symptoms-diagnosis. Accessed March 30, 2021.
10American Lung Association. Bronchoscopy. https://www.lung.org/lung-health-diseases/lung-procedures-and-tests/bronchoscopy. Accessed March 31, 2021.
11American Lung Association. 6-Minute Walk Test. https://www.lung.org/lung-health-diseases/lung-procedures-and-tests/six-minute-walk-test. Accessed April 14, 2021.
12Castro D, Patil SM, Keenaghan M. Arterial Blood Gas. 2021 Jan 27. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan–. PMID: 30725604.
13Davis MD, Walsh BK, Sittig SE, Restrepo RD. AARC clinical practice guideline: blood gas analysis and hemoximetry: 2013. Respir Care. 2013 Oct;58(10):1694-703. doi: https://doi.org/10.4187/respcare.02786. Epub 2013 Jul 30. PMID: 23901131.